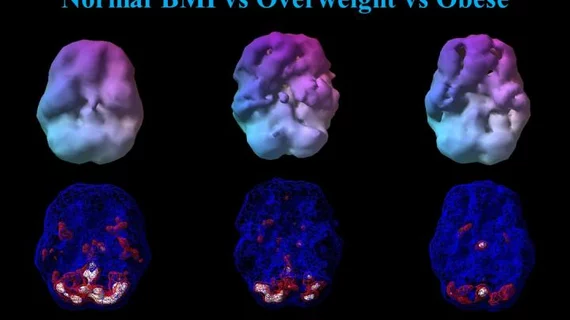
Weight gain and brain dysfunction go hand in hand, according to a large neuroimaging study published Wednesday, sparking concern for the more than 70% of Americans who are overweight.
Amen Clinics, a network of outpatient mental health clinics in the U.S., analyzed more than 35,000 single-photon emission computerized tomography scans to measure brain blood flow and brain activity. They found that as an individual’s body mass index increased, both metrics decreased, particularly in regions vulnerable to Alzheimer’s damage.
Lead researcher Daniel Amen, MD, said the findings are deeply concerning and noted low cerebral blood flow is the top brain imaging predictor for the disorder.
"This study shows that being overweight or obese seriously impacts brain activity and increases the risk for Alzheimer's disease as well as many other psychiatric and cognitive conditions," Amen, who founded the brain health clinics, added in a statement.
With more than 17,000 adults ranging from 18 to 94 years old included in their research, Amen and colleagues said their study is one of the largest to link obesity with brain dysfunction. Participants with BMI distinctions from underweight to morbidly obese were imaged at rest and while performing a concentration task.
As body weight increased, blood flow progressively declined in nearly all regions of the brain. This was true while patients were still and during their cognitive tests.
George Perry, PhD, chair in neurobiology at the University of Texas at San Antonio, called the findings a “major advance” and remarked that patients should know that lifestyle changes can help prevent Alzheimer’s.
Amen echoed that call on Wednesday.
"One of the most important lessons we have learned through 30 years of performing functional brain imaging studies is that brains can be improved when you put them in a healing environment by adopting brain-healthy habits, such as a healthy calorie-smart diet and regular exercise,” he concluded.
Read the entire study published in the Journal of Alzheimer’s Disease here.