Imaging Informatics
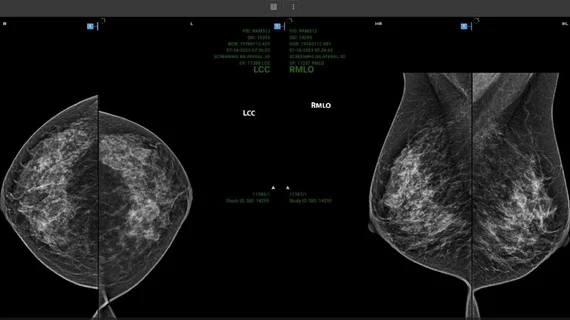
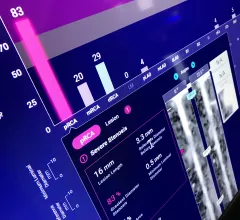
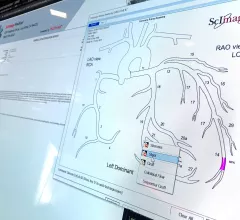
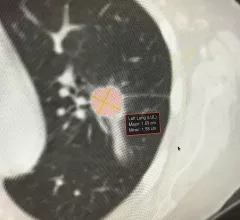
Imaging informatics (also known as radiology informatics, a component of wider medical or healthcare informatics) includes systems to transfer images and radiology data between radiologists, referring physicians, patients and the entire enterprise. This includes picture archiving and communication systems (PACS), wider enterprise image systems, radiology information. systems (RIS), connections to share data with the electronic medical record (EMR), and software to enable advanced visualization, reporting, artificial intelligence (AI) applications, analytics, exam ordering, clinical decision support, dictation, and remote image sharing and viewing systems.