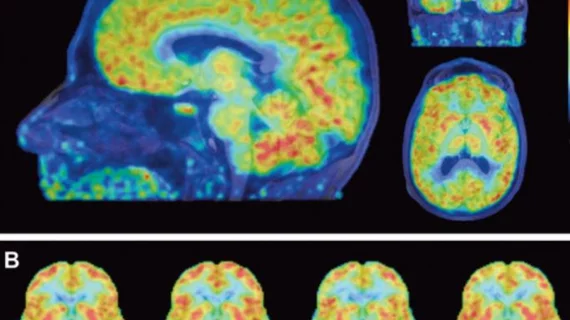
PET imaging may hold promise for personalizing treatment in patients with tuberculosis meningitis (TBM), a rare disease that leaves some survivors with permanent brain damage, reported researchers from Johns Hopkins University School of Medicine in Baltimore.
According to the Dec. 5 study published in Science Translational Medicine, the team tested a uniquely tagged version of the TB drug rifampin to demonstrate how little of it makes its way to TB infection sites in the brain.
“Really precise information has never been easy to come by for how much rifampin gets to any given patient where it’s needed,” said corresponding author Sanjay Jain, MD, in a prepared statement. “We’ve been able to use technology to find that long-needed information about this very troubling disease.”
Jain and colleagues created an “experimentally infected” colony of rabbits with TBM, injected them with the drug [11C]rifampin and tracked its levels in the cohorts’ brains over six weeks. Rabbits were chosen because they display similar TBM symptoms to humans. Following two weeks of treatment, PET imaging showed a decrease in [11C]rifampin’s TBM lesion penetration. The levels of the drug found in the blood fell from 32 to 11 percent.
Importantly, that decrease wasn’t apparent in cerebrospinal fluid (CSF) samples taken, despite CSF’s use in determining drug and infection levels in humans.
Ten adult humans with TBI already receiving rifampin therapy were also given the tagged drug. After undergoing PET scanning, one 24-year-old female showed the drug penetrated infected lesions at a mark of less than five percent.
Jain and colleagues believe their results illuminate why drug treatments for TBM may not be totally effective. PET imaging, they argue, may help ensure enough of the drug is reaching infected TBM areas.
“We used to think we could just give a drug and patients should get better,” Jain said in the statement. “Now, we have tools to measure the nuances that make a difference. PET could be used to study other antibiotics and also allow precision medicine approaches in resource-rich settings, such as the U.S. for other serious infections including MRSA (methicillin-resistant Staphylococcus aureus).”