Human nature being what it is, physician participation in Medicare’s Physician Quality Reporting System (PQRS) will likely accelerate as the agency phases incentives out and penalties in. The effect may prove especially conspicuous since the bonuses have been voluntary and modest. By contrast, the forfeitures will be automatic and, if paired with other pay-for-performance requirements, impossible to ignore.
From where CMS sits, the increasing pressure is necessary medicine. The latest crunched data on PQRS participation, recorded in 2010, showed fewer than 20 percent of eligible physicians satisfactorily reporting in. Newer estimates suggest a current join rate in the neighborhood of 30 percent, but even that would land below the levels CMS surely hoped to reach by now.
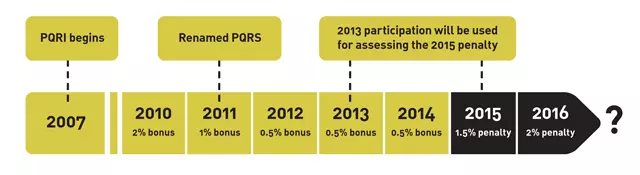
The agency launched PQRS in 2007 as a 2 percent bonus system to facilitate a quality-reporting provision in the Tax Relief and Health Care Act. It will stop paying the current bonus, 0.5 percent, in 2014. The next year it will levy a 1.5 percent deduction—assessed on failure to participate as of 2013—followed by a hike to 2 percent in 2016. The program remains voluntary, but figure in the likelihood that Medicare reimbursements will continue to fall, and the agency’s point on PQRS is clear: Show your quality or forfeit your profitability.
For nuclear radiologists hoping to avoid the pay cut, the ramp-up period is going to have to be quick, condensed—and, in many cases, unenthusiastic.
“I don’t have any hard numbers, but I do know that very few of our members are currently participating,” says Gary Dillehay, MD, referring to the rolls of the professional association of which he is president, the Society of Nuclear Medicine and Molecular Imaging (SNMMI). “Most of us who practice just nuclear medicine have not found PQRS to be [clinically] useful, and it takes more time and effort than it’s worth for any sort of financial return.”
Dillehay, who practices in Chicago and teaches at Northwestern University’s Feinberg School of Medicine, says part of the problem owes to the difficulty of tying imaging to outcomes since diagnostic radiologists don’t have their own patients. Performance measures end up reflecting how consistently processes get reported rather than, say, how appropriately patient studies are conducted or how skillfully images are read. Dillehay adds that he had a role in the initial process of selecting PQRS indicators specific to nuclear medicine. “We suggested three or four,” he recalls, “but the only one that made it in calls for documenting that you compared the study you’re reading with prior studies in the report.”
Despite PQRS’s lack of attractiveness to nuclear medicine specialists and radiologists, the field must adapt to the changing face of reimbursement. After all, it’s not going away, says Dillehay. He encourages participation sooner rather than later and touts a way in that may prove a stronger motivator than the approaching penalties: the potential to tie PQRS reporting to that for Maintenance of Certification (MOC) requirements. “If people can do both at once, it may make things a lot easier,” Dillehay says.
“The government is moving toward demanding quality reporting if they’re going to pay us for our work,” he says. “That’s not an unreasonable thing for them to ask. The transition may be painful, but it’s probably a good thing overall.”
Inside Higher stakes, better quality
For its part, CMS has clearly strived to make the PQRS system more user-friendly than when the agency first rolled it out as PQRI, the I standing for “Initiative.” Early adopters, most of whom used claims data as their measures, were frustrated by a bonus-denial rate of close to 50 percent, notes Walter McDonald, MD, chief executive of the American Society of Internal Medicine. CMS’ website dedicated to PQRS now offers users the choice of easier reporting through a registry, group practice or the EHR incentive-reporting program. (Satisfying Meaningful Use does not mean satisfying PQRS—the two remain separate.)
McDonald, a former head of the American College of Physicians who now speaks on PQRS participation to groups, is bullish on quality improvement but empathetic with the widespread resistance to PQRS across all specialties. He cites several reasons the program has been slow to catch on, not the least the layer it adds to an already thick tangle of CMS programs, guidelines and requirements. Then too, there’s the simple reality that physicians’ top priority is patient care—and there are only so many hours in a day.
All that acknowledged, McDonald likes the promise PQRS has started to show. “We’re beginning to see some hard data [suggesting] that tying income to quality of care and outcomes does have an impact,” he says. “Quality improves as the stakes increase.” Granting that CMS often fails to comprehend “how burdensome these programs can become,” he adds that smoothing PQRS’ speed bumps will take physicians’ patience—and input. “I’ve found that the bureaucracies are willing to listen. It takes time; it sometimes feels like you have to beat someone over the head with a two by four to get through to them. But eventually they do listen and act on what you tell them.”
Decreasing complexity
In 2012, the Journal of the American College of Radiology published a study showing that only a minority of radiologists successfully qualified for PQRS incentives during the program’s first four years. The good news was that, despite the disappointing showing, the results had improved each year—and radiology was quite well ahead of the curve (a 23.7 percent success rate for radiologists vs. 16.3 percent for nonradiologists).
The study’s lead author, Richard Duszak Jr., MD, chief medical officer of the American College of Radiology’s Neiman Health Policy Institute and an interventional radiologist in Memphis, Tenn., expects the success rate to continue rising along that same trajectory. He points out that medical societies and colleges have stepped up their educational efforts around PQRS and billing companies have gotten up to speed with the tools. “There are still some issues with regard to whether physicians think the metrics are important, but they’re easier to implement in practice,” says Duszak.
Meanwhile, registry reporting has proven more successful than claims-based, and approved PQRS “wizard” applications are making reporting similar to filing taxes through familiar tax-filing programs. “There are a whole lot of things that have made the investment—both on the physician side and the practice side—a lot less than it used to be,” says Duszak.
He offers advice to stragglers, framing it as a question followed by a prediction. “What is 2 percent of your salary?” he asks. “Are you willing to throw that away? And if the program is moving from 2 percent bonuses to 2 percent penalties, it doesn’t take a Las Vegas card shark to foresee that the penalty is not unlikely to go to 3 percent, 4 percent.” His voice trails off. Point taken.