The coronavirus outbreak is pushing hospitals and physicians to their limits, with many forced to adapt on the fly. In the U.K., where cases are on the rise, radiologists at the center of the pandemic have taken it upon themselves to prepare others for what lies ahead.
A group of four U.K.-based chest radiologists shared how their departments have been coping, x-ray exams’ new role, and lessons for radiology departments soon to be slammed with patients. They shared those thoughts in a March 20 opinion piece published in the BMJ.
“This has been a steep learning curve for frontline clinicians,” the authors wrote Friday. “Such is the novel nature of this disease; decision making by clinical radiologists is emerging as one of the key parts of frontline triage.”
Below are three takeaways from Samanjit S. Hare, a consultant chest radiologist with Royal Free London National Health Services Foundation Trust, and colleagues.
Chest x-ray exams are vital
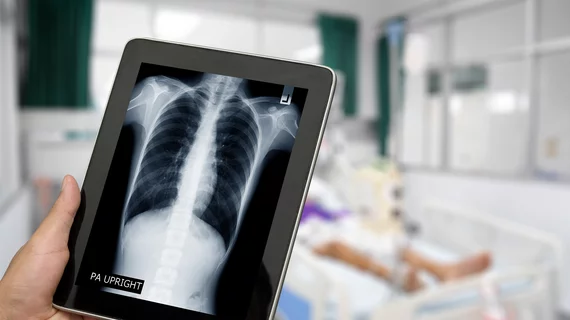
Each patient with suspected COVID-19 who enters a National Health Services-run emergency department receives a blood test and chest x-ray, according to Hare et al.
“Radiologists now find themselves at the frontline of helping to manage the COVID-19 outbreak,” Hare and colleagues wrote. “The chest x-ray has emerged as the frontline diagnostic imaging test…”
Radiology resources are already lacking in the UK, they said, and departments are funneling everything they have toward prioritizing x-ray reporting over other imaging. So far, its helped them quickly determine those with lung infection who likely have the coronavirus.
Importantly, some studies have suggested that x-ray may miss findings indicative of COVID-19 that appear obvious on CT scans.
Computed Tomography sterilization
Hare and colleagues explained ensuring that CT scanning equipment is properly sterilized is becoming a “real issue.”
Radiologists imaging patients with severe symptoms are being forced to review such scans while patients remain on the exam table. This helps determine whether equipment will likely need a deep clean or a shorter wipe-down, they said.
In some cases, individuals not suspected to have the new virus are sent for a scan, only to have the results suggest otherwise. When possible, physicians should wait until a lab test confirms a coronavirus diagnosis before examining more stable patients.
“This is so radiologists can decide if the CT scan should take place on the ‘COVID CT scanner’ or the nominated ‘clean’ CT scanner, thereby reducing the potential risk of contamination and further spread of infection,” the authors wrote.
Protecting valuable radiology workforce
An estimated 20% of the NHS workforce is likely to require self-isolation at some point, and radiology departments must prioritize safeguarding staff with personal protective equipment to avoid worst-case scenarios.
“With frontline clinicians now relying on rapidly reviewed chest x-rays to appropriately triage the sickest patients (whilst awaiting diagnostic PCR tests), this would add even more burden to an overstretched system,” they commented.
Hare and colleagues at the NHS published an opinion piece about the pandemic two weeks ago predicting some of these problems. They also considered using CT as a frontline tool to diagnose the virus.
As of March 23, there are more than 350,000 cases across the globe, with more than 15,000 deaths and upward of 100,000 recoveries.